Anal Yeast Infection – Causes, Symptoms, and Treatment of Rashes, Inflammation, and More
A yeast infection in the anal area, a rash on the buttocks, or inflammation of the anus —discomforts in this area are unpleasant and a sensitive topic for many men. Yet problems such as a sore butt, pimples between the buttocks, or pain in the anal area are common and easily treatable. The key is to correctly identify the cause and act early. In this guide, we explain what’s behind typical anal complaints, what risks may arise, and what you can do for treatment and prevention.
What is a yeast infection in the anal area?
A yeast infection in the anal area (medically known as anal candidiasis or perianal candidiasis) is a fungal infection affecting the anus and the surrounding skin. It is usually caused by yeast fungi of the genus Candida, which are naturally present on the skin and in the intestines. Under certain conditions—such as moisture, heat, or a weakened immune system—they can multiply uncontrollably and trigger an infection. Anal yeast infections are more common in adults than is often assumed and occur equally in men and women.
Symptoms: How can I tell if I have a yeast infection in the anal area?
Common symptoms of an anal yeast infection include:
- Severe itching around the anus and between the buttocks
- Redness, irritation, and inflammation around the anus
- Sore Buttocks – Sore, Irritated Skin Around the Anus
- Burning or pain in the anus, especially during bowel movements
- Rash on the buttocks or around the anus (widespread redness, weeping areas)
- White patches or flaky skin in the anal area
- Sores around the anus that heal poorly or not at all
GenitPlus - Anti-inflammatory intimate care
GenitPlus Oil-Based GenitPlus makes it easier to clean your intimate area and helps prevent problems. Ideal for acute discomfort in the intimate area
Antibacterial thanks to tea tree oil
Especially for the male intimate area
Developed by urologists and dermatologists
- Regular price
-
CHF 23.80 - Regular price
-
- Selling price
-
CHF 23.80








Rash on the buttocks: a fungal infection or something else?
Not every rash on the bottom is caused by a fungal infection. Similar symptoms can also be caused by other factors—such as intertrigo (skin rash), eczema on the buttocks, contact dermatitis, or bacterial infections. Pimples between the buttocks can also indicate clogged sebaceous glands, ingrown hairs, or a coccyx fistula. An accurate diagnosis is important in order to initiate the correct treatment.
Pimples between the buttocks
Pimples between the buttocks are often caused by friction, sweating, and poor ventilation in that area. Clogged pores, ingrown hairs, or inflamed sebaceous glands are common triggers. In rare cases, they may also indicate a pilonidal cyst (sinus pilonidalis) or a bacterial infection. If you have persistent or painful pimples between the buttocks, you should see a doctor.
Eczema on the buttocks
Eczema on the buttocks (also known as anal eczema or perianal eczema) is an inflammatory skin condition in the anal area characterized by severe itching, redness, and flaking. It can be triggered by allergies, contact with irritants (e.g., wet wipes, soaps), chronic conditions such as Crohn’s disease, or fungal infections. Eczema on the buttocks that does not respond well to simple hygiene measures should be evaluated by a dermatologist.
Risks and Causes of Anal Yeast Infections and Anal Discomfort
There are many causes of anal discomfort. Fungal infections, inflammation, and rashes on the buttocks are usually caused by a combination of several factors. Understanding these causes is the first step toward effective prevention.
Moisture and poor ventilation
Due to its anatomical location between the buttocks, the anal area is particularly prone to moisture buildup. Sweating, not drying off thoroughly after showering, or wearing tight-fitting synthetic underwear can contribute to a moist environment. Moisture and warmth create ideal conditions for fungi and bacteria—which can lead to a yeast infection around the anus, a sore bottom, or anal inflammation.
Friction and mechanical irritation
Friction between the buttocks—whether from walking, exercising, or cycling—can irritate and damage the skin in the anal area. A compromised skin barrier is more susceptible to fungal and bacterial infections. Excessive or harsh cleaning with toilet paper or scented wipes can also irritate the sensitive skin around the anus and lead to a rash in that area.
Inappropriate cleaning products
Many commercially available soaps, shower gels, and wet wipes contain fragrances, preservatives, and harsh surfactants that can irritate the sensitive skin around the anus. This can lead to anal inflammation, itching, or eczema on the buttocks. Specially formulated, pH-neutral intimate cleansers are much better suited for cleaning the anal area.
A weakened immune system and antibiotics
A yeast infection in the anal area often occurs after taking antibiotics. Antibiotics kill not only harmful bacteria but also the beneficial bacteria that normally keep yeast growth in check. This upsets the balance of the natural gut flora, allowing fungi such as Candida to multiply unchecked. A weakened immune system due to stress, illness, or diabetes also increases the risk of an anal yeast infection.
When should you see a doctor?
The following symptoms should be evaluated by a doctor:
- Severe pain in the anus, especially during bowel movements
- Bleeding in the anal area
- Sores around the anus that won't heal or are getting worse
- Persistent rash on the buttocks despite improved hygiene
- Fever or general feeling of illness
- Recurrent fungal infections in the anal area

Treatment and Prevention of Anal Yeast Infections and Anal Discomfort
Treatment for anal discomfort depends on the underlying cause. While mild cases of a sore bottom or a rash on the buttocks can often be managed with improved hygiene and appropriate care products, a fungal infection or bacterial inflammation of the anus requires targeted medical treatment. Prevention is always the best approach.
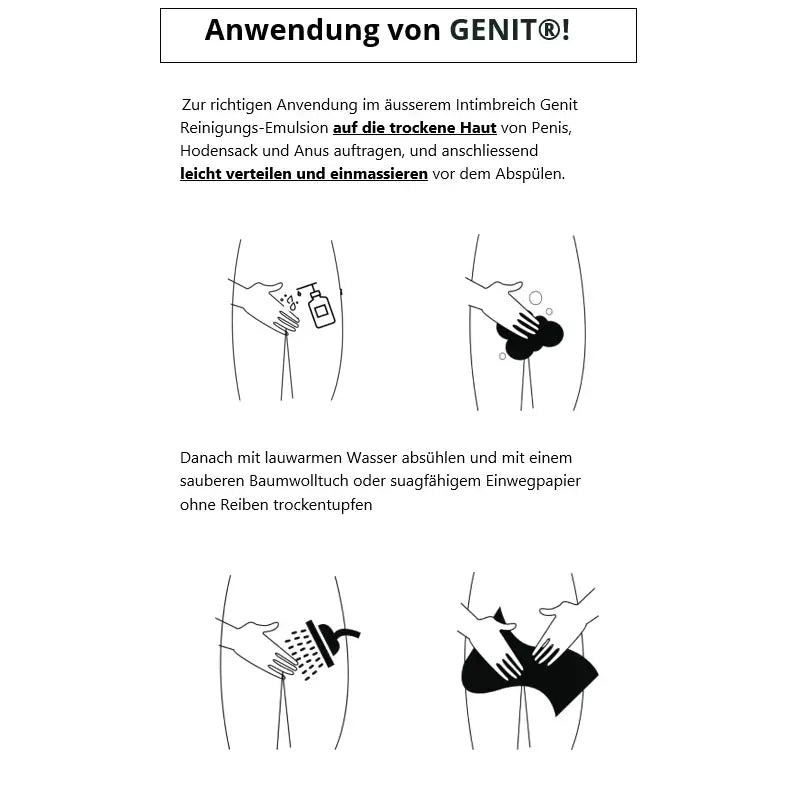
Proper Cleaning of the Anal Area
Careful yet gentle cleansing of the anal area is the most important step in preventing and treating anal discomfort.
The key is to be thorough but gentle—aggressive cleansing can irritate the skin and make the condition worse. Use lukewarm water and a pH-neutral cleansing emulsion specifically designed for the intimate area. Perfumed soaps and wet wipes should be avoided, as they can irritate the sensitive skin around the anus.
Step-by-step cleaning:
- Gently clean the anal area with lukewarm water after a bowel movement
- Use a special intimate wash (not regular shower gel)
- Gentle, circular motions – no aggressive scrubbing
- Rinse thoroughly – no residue left on the skin
- Gently dab with a soft cloth or cotton pad—do not rub
- Let the area dry thoroughly—moisture promotes fungal growth
Treating Anal Fissures: Self-Care Measures
If you have a sore bottom or anal discomfort without a clear fungal infection, the following measures may provide relief:
- Wear loose-fitting, breathable cotton underwear
- Avoid synthetic fabrics and tight clothing
- Shower after exercising and dry your genital area
- Avoid using scented wet wipes and harsh toilet paper
- Use a specially formulated intimate cleanser for the anal area
- If you suspect a fungal infection: do not use conventional cortisone creams, as they can promote fungal growth
Recommended products: Intimate cleansers for the anal area
For daily cleansing and care of the anal area, we recommend a specially formulated intimate cleanser that is gentle, pH-neutral, and free of harsh surfactants and fragrances. GENIT developed a micellar oil-based cleansing emulsion recommended by urologists and dermatologists for male intimate care. The gentle formula helps cleanse thoroughly without drying out the skin or disrupting the natural microbiome.
GenitMEN - Cleansing emulsion for daily use
GenitPlus Oil-Based GenitPlus makes it easy to clean your intimate area. Perfect for your daily shower routine.
Antibacterial thanks to tea tree oil
Especially for the male intimate area
Developed by urologists and dermatologists
- Regular price
-
CHF 22.80 - Regular price
-
- Selling price
-
CHF 22.80





Prevention: How to Keep Your Anal Area Healthy
Prevention is the best treatment. These simple steps can significantly reduce the risk of anal yeast infections, rashes on the buttocks, and anal inflammation:
- Gentle daily cleansing with a pH-neutral intimate wash
- Make sure to dry the anal area thoroughly after washing and after exercising
- Wear breathable underwear made from natural fibers
- Take probiotics to support your gut flora after taking antibiotics
- Boosting the immune system: a balanced diet, enough sleep, and stress reduction
- If symptoms recur: Do not delay seeking medical attention
Frequently Asked Questions About Anal Yeast Infections
How long does it take for a yeast infection around the anus to heal?
With the right antifungal treatment, symptoms usually improve within a few days. Complete healing generally takes 1–2 weeks. However, treatment should be continued until the end, even if symptoms subside earlier—otherwise, a relapse may occur.
What is the difference between a yeast infection around the anus and hemorrhoids?
Hemorrhoids are enlarged blood vessels in the anal area that can cause itching, burning, and occasional bleeding. A fungal infection in the anal area causes similar symptoms but is often accompanied by more pronounced redness, flaking, and whitish patches. A medical examination is necessary to distinguish between the two with certainty.
Why won't a wound on my butt heal?
A sore on the buttocks that won't heal can have various causes: a chronic fungal or bacterial infection, eczema, a fistula, or even a skin condition such as psoriasis. If a sore on the buttocks doesn't heal despite proper care and hygiene, you should see a doctor or dermatologist as soon as possible.
















